Highmark Prior Auth Form
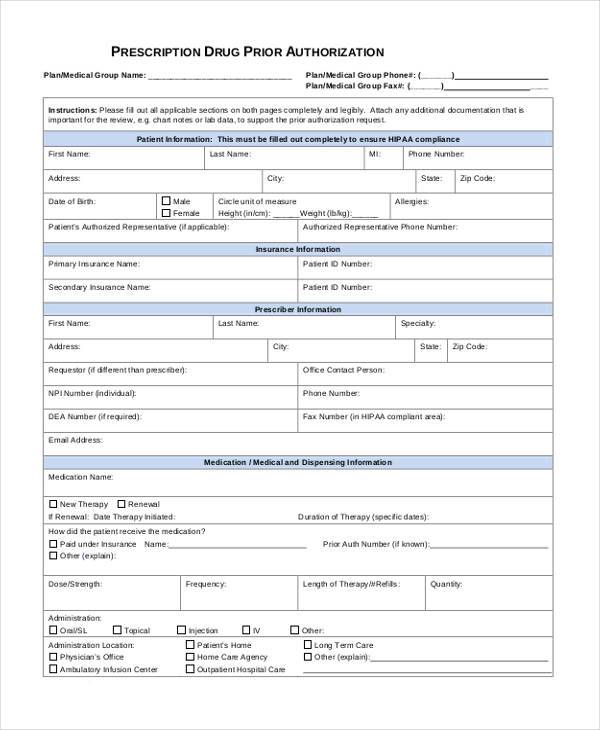
Highmark Prior Auth Form - Designation of authorized representative form. Picture_as_pdf applied behavioral analysis (aba) prior authorization request form. Cymbalta, lyrica, savella) testosterone therapies miscellaneous items: Web prior authorization below is a list of common drugs and/or therapeutic categories that require prior authorization: Durable medical equipment over $500. Any service that requires an authorization from a primary payer, except nonexhausted original medicare services. The authorization is typically obtained by the ordering provider. All inpatient admissions, including organ transplants. Web prior authorizations are required for: A physician must fill in the form with the patient’s member information as well as all medical details related to the requested prescription.
Web prior authorization request form highmark health options is an independent licensee of the blue cross blue shield association, an association of independent blue cross blue shield plans. Web prior authorizations are required for: Request for prescription medication for hospice, hospice prior authorization request form pdf form medicare part d prescription drug claim form The authorization is typically obtained by the ordering provider. Picture_as_pdf durable medical equipment (dme) prior authorization request form. Use this form for all physical, occupational, speech, and feeding therapies, pulmonary and cardiac rehabilitation, and chiropractic care. Agents used for fibromyalgia (e.g. General provider forms & references after hours services betterdoctor provider faq carc and rarc. Any service that requires an authorization from a primary payer, except nonexhausted original medicare services. Web a highmark prior authorization form is a document used to determine whether a patient’s prescription cost will be covered by their highmark health insurance plan.
Cymbalta, lyrica, savella) testosterone therapies miscellaneous items: General provider forms & references after hours services betterdoctor provider faq carc and rarc. All inpatient admissions, including organ transplants. Web prior authorization request form highmark health options is an independent licensee of the blue cross blue shield association, an association of independent blue cross blue shield plans. Request for prescription medication for hospice, hospice prior authorization request form pdf form medicare part d prescription drug claim form Web a highmark prior authorization form is a document used to determine whether a patient’s prescription cost will be covered by their highmark health insurance plan. Web medicare part d hospice prior authorization information use this form to request coverage/prior authorization of medications for individuals in hospice care. Designation of authorized representative form. Durable medical equipment over $500. Web prior authorization below is a list of common drugs and/or therapeutic categories that require prior authorization:
Free Highmark Prior (Rx) Authorization Form PDF eForms
Designation of authorized representative form. Web prior authorization below is a list of common drugs and/or therapeutic categories that require prior authorization: The authorization is typically obtained by the ordering provider. Web prior authorizations are required for: Picture_as_pdf applied behavioral analysis (aba) prior authorization request form.
About Privacy Policy Copyright TOS Contact Sitemap
Web prior authorization request form highmark health options is an independent licensee of the blue cross blue shield association, an association of independent blue cross blue shield plans. Contraceptives, provigil, immediate release fentanyl products specialty drugs (e.g. Designation of authorized representative form. A physician must fill in the form with the patient’s member information as well as all medical details.
4D Result Printable Fill Out and Sign Printable PDF Template signNow
All inpatient admissions, including organ transplants. Web a highmark prior authorization form is a document used to determine whether a patient’s prescription cost will be covered by their highmark health insurance plan. Cymbalta, lyrica, savella) testosterone therapies miscellaneous items: Designation of authorized representative form. Web prior authorization request form highmark health options is an independent licensee of the blue cross.
Gallery of Highmark Bcbs Medication Prior Authorization form Best Of
Web prior authorization below is a list of common drugs and/or therapeutic categories that require prior authorization: Request for prescription medication for hospice, hospice prior authorization request form pdf form medicare part d prescription drug claim form Picture_as_pdf durable medical equipment (dme) prior authorization request form. General provider forms & references after hours services betterdoctor provider faq carc and rarc..
Form ENR187 Download Printable PDF or Fill Online Disabled Child
Picture_as_pdf durable medical equipment (dme) prior authorization request form. Web prior authorizations are required for: Cymbalta, lyrica, savella) testosterone therapies miscellaneous items: General provider forms & references after hours services betterdoctor provider faq carc and rarc. Agents used for fibromyalgia (e.g.
Highmark Enrollment Form Fill Out and Sign Printable PDF Template
Web prior authorization below is a list of common drugs and/or therapeutic categories that require prior authorization: Picture_as_pdf applied behavioral analysis (aba) prior authorization request form. General provider forms & references after hours services betterdoctor provider faq carc and rarc. Any service that requires an authorization from a primary payer, except nonexhausted original medicare services. Some authorization requirements vary by.
FREE 42+ Blank Authorization Forms in PDF Excel MS Word
Contraceptives, provigil, immediate release fentanyl products specialty drugs (e.g. The authorization is typically obtained by the ordering provider. Some authorization requirements vary by member contract. Any service that requires an authorization from a primary payer, except nonexhausted original medicare services. Use this form for all physical, occupational, speech, and feeding therapies, pulmonary and cardiac rehabilitation, and chiropractic care.
Prior Auth Form For Medicare Universal Network
Web prior authorization request form highmark health options is an independent licensee of the blue cross blue shield association, an association of independent blue cross blue shield plans. Durable medical equipment over $500. Use this form for all physical, occupational, speech, and feeding therapies, pulmonary and cardiac rehabilitation, and chiropractic care. Inpatient and outpatient authorization request form. The authorization is.
Request For Prior Authorization Form Proton Pump Inhibitors
Inpatient and outpatient authorization request form. Durable medical equipment over $500. Use this form for all physical, occupational, speech, and feeding therapies, pulmonary and cardiac rehabilitation, and chiropractic care. Web prior authorization request form highmark health options is an independent licensee of the blue cross blue shield association, an association of independent blue cross blue shield plans. Web a highmark.
Kemper Life Insurance Claim Form
Any service that requires an authorization from a primary payer, except nonexhausted original medicare services. Web highmark requires authorization of certain services, procedures, and/or durable medical equipment, prosthetics, orthotics, & supplies (dmepos) prior to performing the procedure or service. All inpatient admissions, including organ transplants. Web prior authorization below is a list of common drugs and/or therapeutic categories that require.
General Provider Forms & References After Hours Services Betterdoctor Provider Faq Carc And Rarc.
Use this form for all physical, occupational, speech, and feeding therapies, pulmonary and cardiac rehabilitation, and chiropractic care. Picture_as_pdf durable medical equipment (dme) prior authorization request form. Web a highmark prior authorization form is a document used to determine whether a patient’s prescription cost will be covered by their highmark health insurance plan. All inpatient admissions, including organ transplants.
Web Medicare Part D Hospice Prior Authorization Information Use This Form To Request Coverage/Prior Authorization Of Medications For Individuals In Hospice Care.
Designation of authorized representative form. Web prior authorization request form highmark health options is an independent licensee of the blue cross blue shield association, an association of independent blue cross blue shield plans. Contraceptives, provigil, immediate release fentanyl products specialty drugs (e.g. Cymbalta, lyrica, savella) testosterone therapies miscellaneous items:
Durable Medical Equipment Over $500.
Request for prescription medication for hospice, hospice prior authorization request form pdf form medicare part d prescription drug claim form Any service that requires an authorization from a primary payer, except nonexhausted original medicare services. Web prior authorizations are required for: A physician must fill in the form with the patient’s member information as well as all medical details related to the requested prescription.
Picture_As_Pdf Applied Behavioral Analysis (Aba) Prior Authorization Request Form.
Agents used for fibromyalgia (e.g. Web prior authorization below is a list of common drugs and/or therapeutic categories that require prior authorization: Some authorization requirements vary by member contract. The authorization is typically obtained by the ordering provider.